{Disclaimer: I can only speculate what misconceptions other people have about psychosis. To be blunt, I thought ‘psychotic’ described a state of being in a romantic relationship, with the sign of someone being psychotic being “sending a whole bunch of texts to a significant-other without reply, and with the other person, and other people if they were to see those texts, not understanding where you’re coming from”. I thought ‘schizophrenic’ described “A middle-aged homeless man talking to himself on public transportation or on the street.” I didn’t recognize when my mind was overpowered with delusions in first-episode psychosis (I behaved on the premises that my beliefs were mostly true), and that these delusions were symptoms of psychosis.}
Here is some information that I didn’t know prior to experiencing psychosis that I think could be common misconceptions:
Misconception: Hallucinations are a “requirement” for someone to be in psychosis.
Reality: Schizophrenia is associated with myriad symptoms, of which hallucinations can be but do not have to be required for a diagnosis.
Some people experience psychosis without ever the most stereotypical symptoms of schizophrenia. I never experienced any form (visual, auditory, olfactory, gustatory, tactile) of hallucination in first-episode psychosis, which lasted >~978 days for me before it was identified by psychiatrists. After, I was involuntarily given antipsychotics, which subsided my symptoms.
Misconception: Psychosis is black-and-white; all-or-nothing.
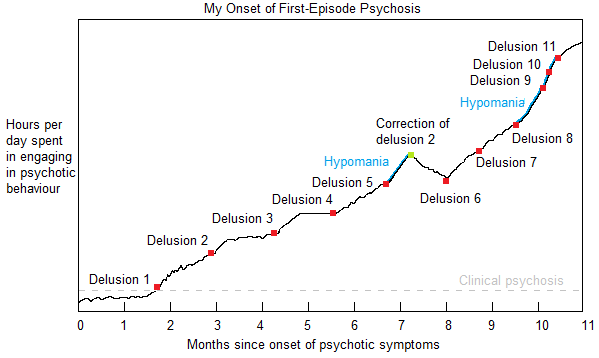
Reality: Psychosis is a state that you slip into, with the onset being different from the peak.
Like how the sky must go through sunset while transitioning from day to night, psychosis is experienced not as a light switch flicking off, but as a descent in which symptoms are experienced more and more frequently. Likewise, one might experience being buzzed, and then tipsy, before being drunk. And one might experience being slightly more conscious after experiencing REM sleep, before being fully awake.
This is (somewhat arbitrarily) what the onset of first-episode psychosis was like for me:
Moreover, you can be at higher risk for a psychotic disorder than the general population, and never develop a psychotic episode. And being higher risk, like having a psychotic disorder, has implications on cognition – decreasing areas such as working memory, attention, coding, processing speed, and executive functioning relative to the general population, while still being higher than the schizophrenic population.
You can also be going through life as someone with your schizophrenic genes, also known as the prodromal phase, before developing first-episode psychosis.
Misconception: Delusions do not feel enlightening.
Reality: Delusions can feel like sudden wonderful realizations, revelations, or epiphanies.
They can feel like you are the one seeing the light. Having delusions feel like looking at photographs with not just the dates written on the backs of them, but paragraphs of text written explaining the meaning behind the images as well. Delusions can feel like complex storylines — based on things that can realistically happen, or have happened (e.g., things prior to your birth that you did not witness firsthand).
Delusions and the behaviour they incite may feel like more extreme versions of behaviour the individual already is known to exhibit. During FEP, I felt compelled to share the content of delusions with others, with the aim of sharing what I believe at the time to be valuable information to improve their lives and/or my life.
The specific delusions and their associated behaviour may vary based on one’s values, personality, interests, chronological life history / circumstances, and comorbid psychiatric conditions.
Misconception: Delusions do not produce on average more powerful emotional experiences than regular beliefs in which you’re mistaken.
Reality: Delusions do the above; they can be accompanied by VERY strong emotions, which could be part of what prompts urgent actions based on delusions.
There are emotions that I’ve only experienced during delusions — these being rage (which I thought was not necessary previously as a term; that anger was enough, for I had not experienced the intensity and directness that was rage before), and hatred. My delusions have also made me feel a shitton of other emotions, including surprised, devastated, shocked, angry, disgusted, fearful, frightened, joyful, hopeful, proud, and purposeful.
Episodes of psychosis can coincide alongside episodes of hypomania or mania.
Misconception: Being psychotic means you care incapable of engaging in the act of planning for a future.
Reality: Capacity for planning, being methodological, and being goal-oriented in hopes of / belief that there is a future with multiple possible outcomes does not contraindicate the presence of psychosis.
It is possible to thoroughly examine delusions, to recall various events in one’s life history, and to journal about one’s life, as well as to plan a trajectory ahead based on delusions, during psychosis.
When I am undergoing psychosis, my actions tend to be more haphazard; I’m more impulsive, and less inhibited. However, my behaviour is not inexplicable to myself: most actions (e.g., novel ways of arranging objects in a bedroom) are planned, and have continuity into time and space (e.g., if on vacation in a different country, similar behaviours continue happening there, and then, due to the self still holding certain beliefs).
Psychosis is not mutually exclusive with never being in a state of planning for months or years or even decades into the future. E.g., I prolifically made Google Documents meant to be shown to various persons several months later, decided on a career to pursue, applied to (and was accepted into) two schools — including the writing of a Special Considerations letter, and decided on a country to live in during first-episode psychosis.
Misconception: The only difference between thoughts in psychosis, and thoughts outside psychosis, is that thoughts during psychosis are mostly false.
Reality: If one is having delusions, one typically does experience a higher frequency of false beliefs (especially during FEP IME) — however, one may not be having delusions all the time, and sometimes the difference, is that thoughts are felt differently.
Sometimes, thoughts feel more intense, muddled, hazier, denser, and/or foggier. Sometimes they feel urgent, scattered, and/or racing. It’s like the difference between writing something barely legible one busy morning, and writing in very standardized handwriting when you have more time that afternoon. If you change the font from Tahoma to Papyrus, the Papyrus thoughts would be neither more or less wrong.
Misconception: People in psychosis exhibit signs that they are in psychosis 100% the time.
Reality: Things done in psychosis look to varying degrees of “psychotic” — including not at all at times.
You aren’t exhibiting signs that indicate overt psychotically all the time to yourself, and those around you, while you’re in psychosis — only noticing signs a % of the time is enough to indicate psychosis.
There are symptoms an outside observer might not guess are happening based on an individual’s behaviour. I rarely experience word salad, and don’t always have difficult-to-comprehend i.e., impaired writing in psychosis. You can do normal activities like walk the dog during psychosis, and be completely unnoticed by strangers that you are currently psychotic.
Looking at photos of me taken by others when I was in psychosis, I don’t think there’s any way from looking at me to tell what I was experiencing. I don’t even think I had more impaired hygiene or self-care during psychosis; I had a harder time with it during spells of depression at ages 19-22 (inclusive) before psychosis. Some photography and videography that I took on my phone were the results of delusions I had, and I now interpret as signs of psychosis, however some photographs and videos are of phenomena I would take outside of psychosis.
Misconception: You need to know a relative diagnosed with schizophrenia to develop psychosis.
Reality: You do not need a relative diagnosed with schizophrenia to develop psychosis.
It is not only schizophrenia (or schizoaffective disorder i.e., schizophrenia + mood disorder over a certain % of the time) that increases the risk of a relative having schizophrenia. They can be framed as belonging in the broader categories — “psychotic disorders” and “schizophrenia spectrum disorders”. Schizotypal personality disorder, schizoid personality disorder, schizophreniform disorder, are some examples of some schizophrenia spectrum disorders in which the sufferer carries genes with greater risk for schizophrenia than the general population.
Of course, what you know about your relatives is limited by their diagnostic opportunities — including their personal willingness to seek out diagnoses — as well as what enters your personal knowledge.
Misconception: Only mania or depression can occur in episodes; psychosis cannot be episodic.
Reality: Psychosis can occur in episodes, and schizophrenia is over 50% cases episodic.
When I first noticed changes going on in the way I interacted with the world in late 2020, I considered that I was was having an episode of something. I knew that Bipolar II involved episodes, and looked up criteria for the disorder, and then contemplated my chances of currently experiencing an episode of hypomania or mania. But I had believed schizophrenia was marked with few sudden behavioural changes, and was a continuous pattern of behaviour with an earlier age of onset than it actually has. I think knowing the likelihood of psychosis to occur in episodes would have helped me identify my episodes as psychotic (as well as occasionally manic or hypomanic): perhaps I would have looked up the criteria at age 22, as I did for Bipolar II then.
Misconception: Schizophrenia is a lot more common than in males than females.
Reality: In Canada in 2016-2017, of those diagnosed with schizophrenia, 56% were “men” and were 44% “women”.
If you want to witness more POVs from schizophrenic females in media, I recommend watching the YouTube Channel Living Well With Schizophrenia.